About us
Hangzhou Go Top Peptide Biotech Co., Ltd. was founded in 2014, is a national high-tech enterprise specializing in R&D and production of peptides and related derivatives. It is also a governing unit of Polypeptide Branch of China Biochemical and Pharmaceutical Industry Association. At present, the company has a peptide research and development center in Hangzhou, covering an area of more than 4,000 square meters, and two commercial peptide factories in Shangyu and Anji, Zhejiang, with several complete peptide production lines, several sets of large-scale peptide synthesis equipment, imported HPLC analysis and preparation equipment, and equipped with a GMP standard clean laboratory. The company has passed the ISO9001:2015 quality management system certification.
Our Products
-
Oxytocin Acetate;Pharmaceutial Peptide;neuropeptide;Short peptide
-
Frag 17-23,885340-08-9,Frag 17-23 Peptide
-
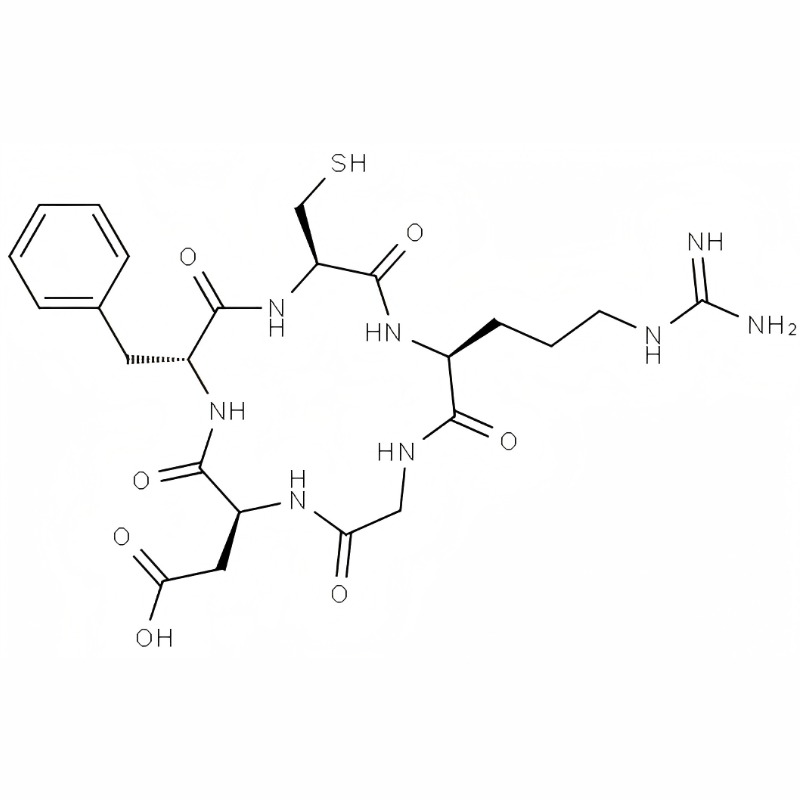
c(RGDfC)/862772-11-0/Synthetic peptide
-
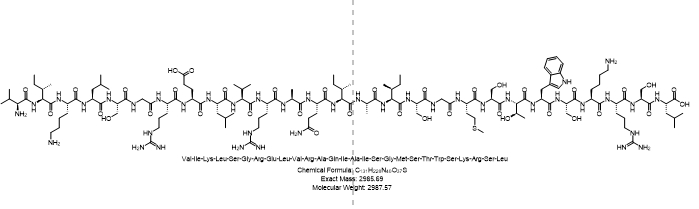
B7-33,(B7-33)H2,B7-33 relaxin
-
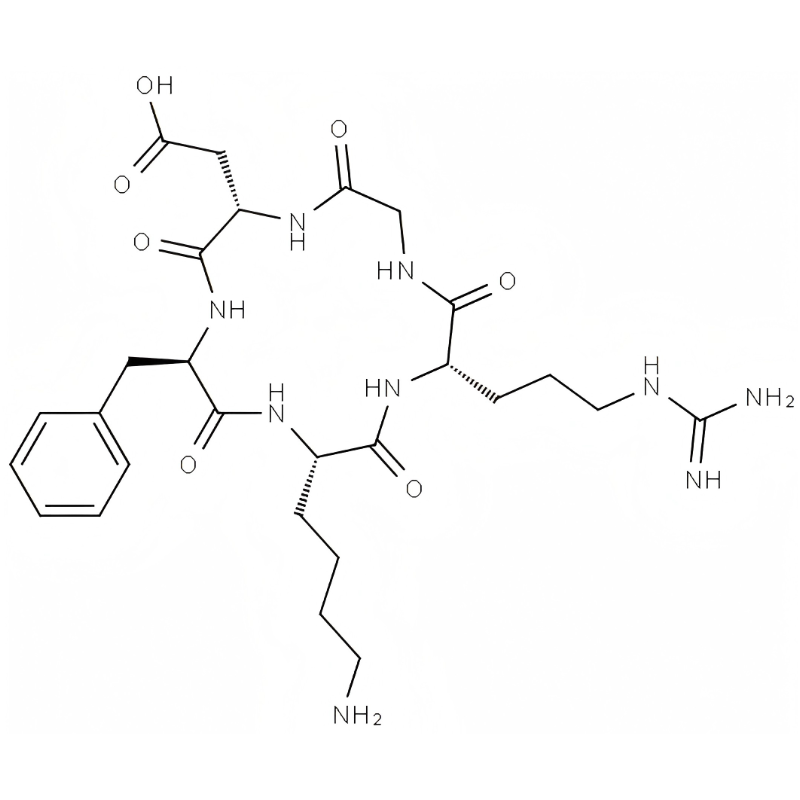
c(RGDfK)/161552-03-0/Peptide analysis
-
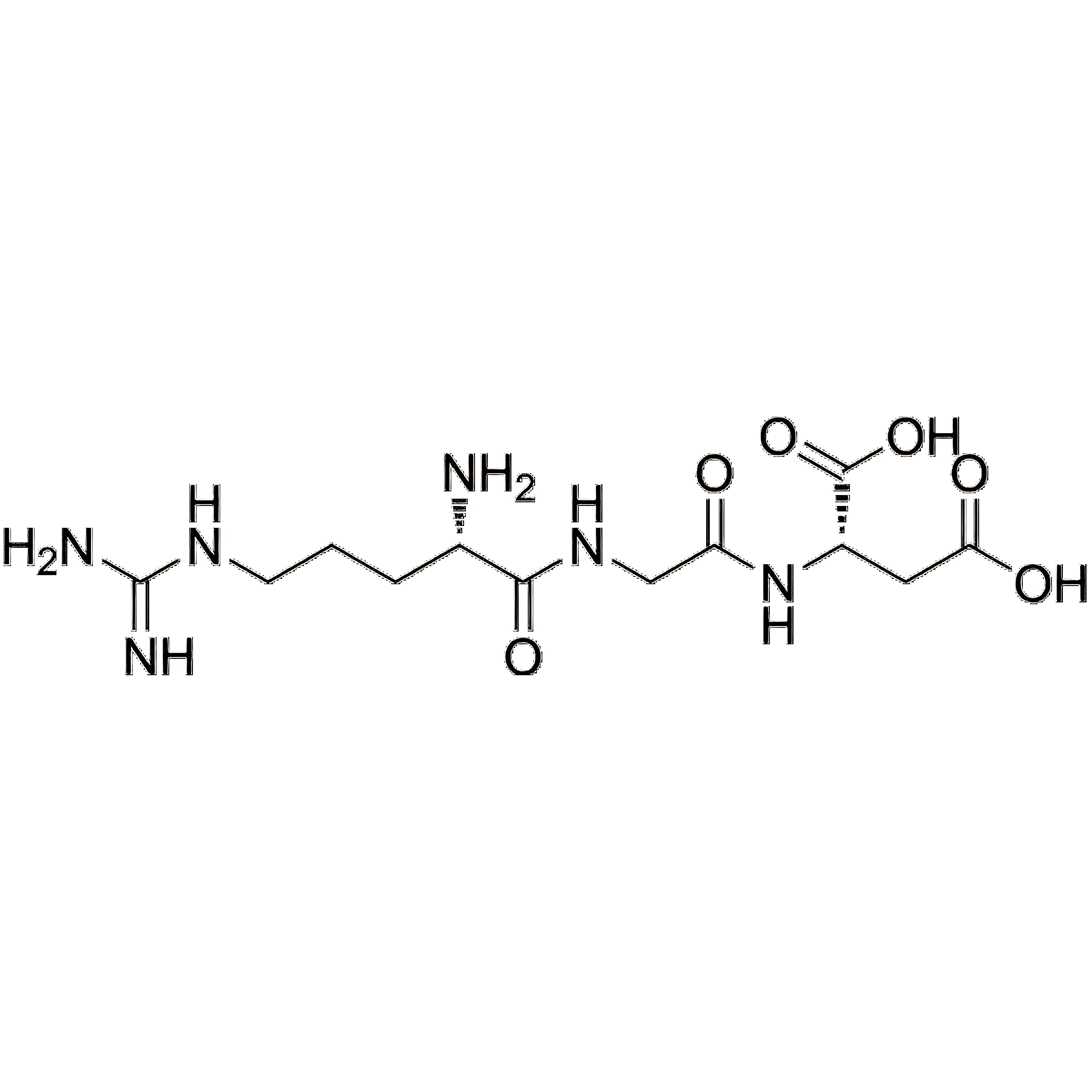
RGD/99896-85-2/Peptide supplier
-
Cyclo(Phe-Val)/14474-71-6/Peptide customization
-
FOXO4-DRI Customized Peptide
-
Customization of High Purity vosoritide
-
High purity peptide PE-22-28